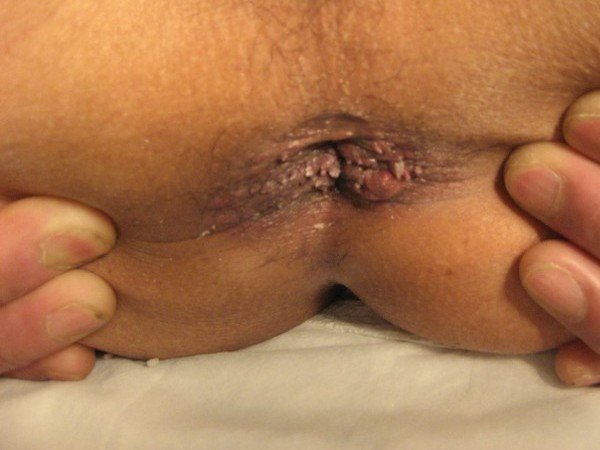
This is the most common sexually transmitted disease. It is estimated that one per cent of adults who are sexually active have warts in the genital or anal area. In the U.S. alone, one million people will develop genital warts each year. Of these, 25 per cent will have recurrent warts. And that is frustrating for the patient and the doctor.
Genital warts are also called condylomata acuminate or venereal warts. The warts are benign and are caused by human papillomavirus (HPV). There are at least 60 types of HPV. Genotypes six and 11 are found in over 90 per cent of cases of genital warts and genotypes 16 and 18 cause cervical cancers.
The virus is transferred from person to person or from contact with something someone has touched. In women, genital warts can grow on the outside or inside of the vagina, on the cervix, in the urethra or around the anus. In men, warts can grow on the tip or shaft of the penis, on the scrotum, in the urethra or around the anus.
How do you get genital warts?
Most, but not all, genital warts are sexually transmitted. Generally speaking warts are more common amongst people whose immune system is poor. But most people who get warts are healthy and well.
How do you know you have genital warts?
Most people with genital warts have no symptoms. By the time a person is infected and by the time the warts appear may be many months or years. The good news is most of those who get infected never develop warts.
The warts are soft fleshy lumps on or near sex organs or anus. Some people have itching or burning. Warts may be hidden in the vagina or anus.
What are the implications of the disease for patients?
The lesions are benign but they do cause psychosocial distress and may affect relationships as the warts are disfiguring and can be transmitted sexually. Genital warts also increase the incidence of cancer in the genital and anal area. Practicing safe sex is important. It is advisable to use barrier protection with new sexual partners. Condoms can reduce the risk of getting genital warts but warts can spread from areas not covered by a condom. Patients who are in stable relationship may not need barrier protection because the partner is already exposed to infection by the time patient sees a doctor.
How do we manage warts?
No specific treatment is appropriate for all patients and a person will need more than one treatment to clear the warts.
Most treatment plans will achieve clearance of virus within one to six months. In 20-30 per cent of patients new warts will occur over months or even years. Patients can treat themselves with podophyllotoxin (0.5 per cent solution or 0.15 per cent cream) and imiquimod (5 per cent cream). Imiquimod is expensive and podophyllotoxin takes longer to cure the condition.
Physicians can treat warts in the office by using trichloroacetic acid or by physical removal using cryosurgery (liquid nitrogen), electrosurgery and excision or laser treatment. In my surgical practice I use electrosurgery and/or excision.
The US Food and Drug Administration (FDA) has approved a new indication for a quadrivalent recombinant vaccine (Gardasil, Merck & Company, Inc) for the prevention of genital warts caused by human papillomavirus (HPV) types 6 and 11 in boys and men aged nine through 26 years. Since the vaccine does not cover all the viruses, about 30 percent of cervical cancers and 10 percent of genital warts will not be prevented by the current vaccines.
The HPV vaccine will not have an impact on an existing infection or any consequences of infection, such as anal and genital warts and cancerous or pre-cancerous changes that you may already have. It is very important to practice safe sex with your partner.
Start reading the preview of my book A Doctor's Journey for free on Amazon. Available on Kindle for $2.99!
hello doctor,
I am 21 male and current have genital warts on penis. What are my chances of gettinganal warts since i have had no anal contact ever?..what are the chances of penile cancer in uncircumsized men with hpv? like me?. I am currently treating my warts and hoping to get rid of these soon . The case is mild since i have 4 warts right now on penis and scrotum. Thank you