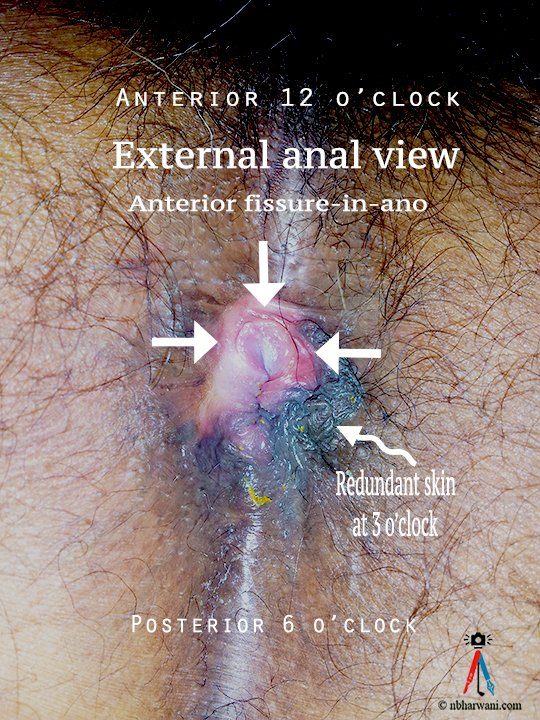
There are various kinds of anal and rectal problems. Some are painful and some are not. Some are serious and others are a mere nuisance – if that is the right word. But all of them are a real pain in the butt – so to speak.
Anal fissure can be really painful. On the other hand, cancer of the rectum may be painless. The only way to find the real diagnosis is to see a doctor to get a good rectal examination consisting of inspection, finger examination and some sort of a scope test depending on your age and history. The important thing is to make sure we are not dealing with cancer or Crohn’s disease.
I have written about this subject before. You can check it out on my website. Today, I want to focus on the management of anal fissure. I want to emphasize that management of painful anal fissure requires a more aggressive approach than managing a “hemorrhoid itch.”
Five steps to manage acute or chronic anal fissure:
1. Make your stool well formed and bulky with a diet high in fiber. Take psyllium (Metamucil) two to four capsules per day with lots of water. This relaxes the anal muscles, helping the healing process.
2. Sit in a hot bath for 20 minutes twice a day for several days until the pain goes away. This really helps the healing process by relaxing the anal sphincter.
3. Minimize the intake of constipating painkillers.
4. Use two per cent diltiazam or nifedipine ointment inside and outside of anal canal twice a day. You need a prescription for this. This medication is associated with healing of chronic anal fissures in 65 to 95 per cent of patients.
5. What can be done if the fissure does not heal after three to six weeks? Rule out other illness of the colon and rectum. Your colon and rectal specialist will advise you on that. Surgical options for treating anal fissure include Botulinum toxin (Botox) injection into the anal sphincter and surgical division of a portion of the internal anal sphincter (partial lateral internal sphincterotomy). Both of these are performed typically as outpatient procedures with good results and minimal of complications.
During my surgical training, I was taught if a doctor does not put a finger in the patient’s rectum then he may end up putting his foot in it. If you have rectal and anal symptoms then get that area examined well. You do not want anybody’s foot in it!
Start reading the preview of my book A Doctor's Journey for free on Amazon. Available on Kindle for $2.99!